The interest of proteins in weight management
Nowadays, obesity is major health problem. In 2018, the WHO (World Health Organization) announced that the number of obesity cases has almost tripled since 1975. In 2016, 13% of adults were obese and 2 out of 5 people were overweight in the world 1.
Obesity and excess weight harm the overall health. They are often associated with many risks: chronic hypertension, type II diabetes, dyslipidemia (abnormal lipid concentration in blood), coronary heart disease, stroke, cancer, musculoskeletal disorders (arthrosis), sleep apnea and other respiratory problems… 1 2
Therefore, weight management, with dietary or overall lifestyle modifications, represents an important challenge for our society. A lot of publications show a great interest in proteins for the loss of fat mass or weight maintenance without muscle mass loss. 2 3 4

How are excess weight and obesity defined?
The WHO uses the Body Mass Index (BMI) to define the overweight status. This is a number which estimate the corpulence using the body weight and the size :5
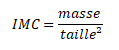
For this calculation, body weight is in kilograms and the size in meter. So, the BMI is expressed in kg/m².
According to the WHO, an adult is overweight when the BMI is greater than or equal to 25 kg/m². He is obese if his BMI is greater than or equal to 30 kg.m². Generally speaking, an ideal BMI is between 18.5 and 25 kg/m².1 5
However, the BMI has some limits since it takes into account the body weight with no consideration of the body composition. That is the reason why a very muscular person can have a BMI greater than 25kg/m² without being overweight. The use of impedance metric measurement methods may appear more relevant. This kind of methods evaluates the lean mass and body fat ratio.
Another limit of the BMI is that it has to be adjusted for people under 18 years old. For them, age have to be considered in the calculation.
What is the interest of proteins in weight management?
Proteins have three interesting properties for weight management2:
- They increase satiety. Therefore, by consuming a certain amount of proteins, we will be satiated more quickly and the overall food intake will be reduced. 2 3
- They increase thermogenesis. As thermogenesis consumes energy, they consequently increase our energy expenditures.2
- They favor muscle gain. This will naturally increase energy expenditures by raising the metabolism since muscles expend energy event at rest. 2 6
However, these phenomena have been recorded in the context of a high protein diet while remaining healthy and balanced. The increase of protein intake alone is not enough.

Do proteins really create more satiety than other nutrients?
Yes they do. Different studies have shown the satiating effect of proteins. 2
Let’s consider a 2005 study, in which 19 people underwent a diet. During the first two weeks, subjects received a traditional diet with the following intakes (in % of total energy): 15% of proteins, 35% of lipids, and 50% of carbohydrates. The two following weeks, food distribution was changing: 30% of proteins, 20% of lipids, and 50% of carbohydrates. During this second period, the 19 people were split into two groups:
- Group A still consumed as much energy in total as during the first 2 weeks, i.e. 2,000kcal ;
- Group B had an ad libitum diet, i.e. they could eat until they were full.
We could imagine that group B might have consumed more calories than group A. However, the exact opposite happened: group B consumed an average of 441 kcal less than group A, which represent a reduction in energy intake of over 22%. This makes possible a weight loss of 4.9kg without hunger during the day or at the end of meals. 8 9
As a conclusion, satiety has increased thanks to proteins.
Then we talked about thermogenesis. What is this? Why increasing it may be helpful for weight management?
Thermogenesis corresponds to the production of heat by the body to maintain us to a certain temperature. For this, the body converts energy into heat. That is why thermogenesis consumes energy.
Certain nutrients naturally increase thermogenesis, especially proteins: there impact on thermogenesis is 2 to 3 times greater than carbohydrates, and up to 10 times higher than fat. 6 10 We often consider that 1g of proteins provide 4kcal to the body (17kJ), but if we subtract from this the energy consumption they generate by thermogenesis, it could be more accurate to say that 1g of proteins provide only 3.1kcal (13kJ). Following this thinking, carbohydrates would represent 3.7kcal/g (15,3kJ/g) instead of 4kcal/g. 2
Regarding the muscle mass gains, why can this be interesting for fat loss or weight maintenance?
Generally, energy expenditures of the average adult depend on three parameters (figure 1): 2
- Basal metabolism, i.e. the amount of energy consumed by the body to simply function,
- Thermogenesis,
- Physical activity.
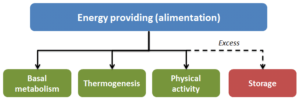
It is commonly believed that it is only possible to act on physical activity. While in reality we can act on all three parameters, even on basal metabolism. Muscles consume energy even at rest. Since it is possible to increase muscle mass, it is therefore possible to increase basal metabolism.
Let’s take an example of 2 subjects which are identical in all points, with the exception that one has 10 more kg of muscles than the other. Basal energy expenditures for this subject will be higher by an average 100 kcal/d. This amount of energy may seem minimal, but let us suppose that a person consumes an excess of 100kcal everyday. After a year, this can represent up to 4.7kg of fat gain. 7
Therefore, it is interesting to consume more proteins to enhance muscle mass building by accompanying it with physical activity. It is also interesting to avoid muscle loss, which would lead to a decrease of the metabolism.
What are the recommended protein intakes to take advantage of these benefits?
The majority of studies which show these benefits were realized with protein intakes twice higher than minimal needs. As a reminder, this corresponds to approximately 12% of total energy intake, i.e. about 0.8g/kg/d. So, quantities used were on average 1.5 to 1,6g/kg/d.
For instance, a study conducted on 65 overweight subjects compared the effect of conventional diet with a high protein diet (twice higher than minimal needs) with the same amount of calories (reducing the amount of carbohydrates to compensate). Diets were energy-restricted so as to enhance weight loss. After 6 months, subjects who followed the high protein diet had lost on average almost twice as much weight (-8.9kg) than the others (-5,1kg). There were no significant changes for the control group. 2 11
However, for overweight people (BMI > 25 kg/m²), it may be preferable to think differently than in g/kg of body weight in order to establish the protein amount to consume daily. Therefore, in 2015, the EFSA submitted a recommendation of approximately 105g of proteins per day for an overweight adult. 12
What proteins should be consumed?
All proteins do not affect satiety, thermogenesis or muscle mass gains with the same impact. This answer will be the topic of our next article, in which we will talk about milk proteins because they are particularly interesting for weight management.

For more information, contact us.
Authors: Rémi Maleterre & Audrey Boulier.
_______________________________________________________________________________________________
[1] « Obesity and overweight». World Health Organization. WHO. February 16, 2018 [consulted: july 09, 2019]. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
[2] D. Paddon-Jones, E. Westman, R.D. Mattes, R.R. Wolfe, A. Astrup, M. Westerterp-Plantenga (2008). Protein, weight management, and satiety. The American Journal of Clinical Nutrition, Volume 87, Issue 5, May 2008, Pages 1558S–1561S. Pub May 01, 2008. https://doi.org/10.1093/ajcn/87.5.1558S
[3] Soenen S., Westerterp-Plantenga, Margriet S. (2008). Proteins and satiety: implications for weight management. Clinical Nutrition and Metabolic Care. Vol 11:6, 747-751. Pub November 2008. https://doi.org/10.1097/MCO.0b013e328311a8c4
[4] Noakes M. (2008). The role of protein in weight management. Asia Pacific Journal of Clinical Nutrition. 17:S1, 169-171. Pub January 2008. https://doi.org/10.6133/apjcn.2008.17.s1.41
[5] Nuttall F.Q. (2015). Body Mass Index. Nutr Today, 50(3):117-128. Epub April 07, 2015. https://doi.org/10.1097/NT.0000000000000092
[6] L. Tappy (1996). Thermic effect of food and sympathetis nervous system activity in humans. Reprod Nutr Dev. 36(4):391-7. Pub 1996.
[7] R.R. Wolfe (2006). The underappreciated role of muscle in health and disease. Am J Clin Nutr. 84(3):475-482. https://doi.org/10.1093/ajcn/84.3.475
[8] A. Astrup (2005) The satiating power of protein – a key to obesity prevention? Am J Clin Nutr. 82(1):1-2. Pub July 2005. https://doi.org/10.1093/ajcn.82.1.1
[9] D.S. Weigle, P.A. Breen, C.C. Matthys, H.S. Callahan, K.E. Meeuws, V.R. Burden, J.Q. Purnell (2005) A high-protein diet induces sustained reductions in appetite, ad libitum caloric intake, and body weight despite compensatory changes in diurnal plasma leptin and ghrelin concentrations. Am J Clin Nutr. 82:41– 8. Pub July 2005. https://doi.org/10.1093/ajcn.82.1.41
[10] Halton T.L. (2004). The effects of high protein diets on thermogenesis, satiety and weight loss : a critical review. Journal of American College of Nutrition, 23(5), 373-385. https://doi.org/10.1080/07315724.2004.10719381
[11] A.R. Skov, S. Toubro, B. Ronn, L. Holm, A. Astrup (1999). Randomized trial on protein vs carbohydrate in ad libitum fat reduced diet for the treatment of obesity. Int J Obes Relat Metab Disord 1999;23:528 –36. Pub May 1999.
[12] EFSA (European Food Safety Authority). Scientific Opinion on the essential composition of total diet replacements for weight control. EFSA Journal 2015;13(1):3957.
The added interest of milk proteins for weight management
As we already mentioned in our previous article “The interest of proteins in weigh management”, the WHO warns populations about the statistics on obesity: over 2 billion people are overweight in the world, and this number is growing every year. 1
We previously insisted on the interest of proteins for weight loss. But among all the protein sources all do not bring the same benefits. Milk proteins, for example, have particularly interesting features for weight management purposes.
How can milk protein be interesting for weight management?
These proteins are interesting for weight management for different reasons.
Proteins in general are very relevant for weight management. At a high concentration, they have an important satietogenic effect and they enhance thermogenesis and muscular mass gains.2 This is valid for all proteins at different levels, as described more precisely in the article “How can proteins be interesting in weight management?”.
Furthermore, there are two types of proteins in milk: whey proteins and micellar caseins; and the latter represents an important source of calcium, whose efficiency to enhance weight loss has been proven. 3 4

Has the efficiency of calcium to enhance weight loss been really proven?
Yes it has, many studies have shown this. We can take the example of a recent study of 2019 in which overweight people (BMI > 25kg/m²) have been put on an energy-restricted diet with moderate physical activity. They were divided into three groups: 5
- Group C was the control group;
- Group S had a supplementation of calcium (1,500mg) and vitamin D (10µg)
- Group D consumed 4 to 5 dairy products per day (in order to provide approximately the same amount of calcium and vitamin D than group S).
Results regarding weight loss are given on figure 1. The group D significantly presents the best results for the circumference of waist, hips and abdomen. However, with regards to the weight loss, the difference will initially seem less impressive. This is due to the fact that group C and S have lost more than only fat mass. After 6 months, group C has lost 2.1kg of lean mass, group S lost 1.7 kg, while group D only lost 1.0kg. Dairy products, a source of calcium, vitamin D and proteins (whey and micellar caseins) allowed a better retention of muscle mass and a more efficient fat loss.5
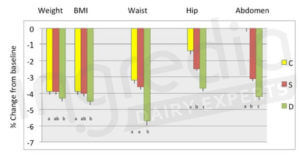
Figure 1: Percentage of changes concerning weight (kg), BMI (kg/m²), waist size (cm), hip size (cm), abdomen size (cm) after 6 months of the diet.5
C: control group (n=30) / S: supplement group (n=37) / D: dairy products group (n=30)
How can calcium enhance weight loss?
To understand this process, we need to detail certain aspects of calcium metabolism.
Calcium has an important role in fat cells. It has been shown that an increase of calcium concentration in these cells would increase fat accumulation (lipogenesis) and inhibit fat degradation (lipolysis).The calcium concentration in cells is regulated by parathyroid hormone and the active form of vitamin D (1,25-hydroxy vitamin D). This is described in figure. 2 6
The hormone activity is regulated by dietary calcium. As a matter of fact, it can suppress the activity of these hormones. Consequently, this could reduce the calcium entry in fat cells, thus significantly reducing fat accumulation while having the opposite effect of enhancing lipids degradation (figure 3). 6 7
In other words, increasing calcium consumption would limit fat storage and act as a natural fat burner. A 2003 study has shown that a high calcium diet could multiply fat degradation by an average of 3 to 5. 6 7
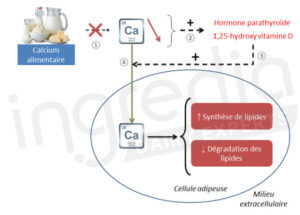
Figure 2: Effect a diet below calcium requirements on lipid metabolism
① Lack of dietary calcium in the extracellular environment
② Activation of the parathyroid hormone and the active form of vitamin D (1,25-hydroxy vitamin D).
③ Stimulation of calcium entry in fat cells
④ Calcium entry in fat cells which enhance fat synthesis and inhibit fat degradation
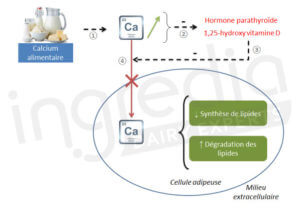
Figure 3: Effect of a diet high (greater than or equal to needs) in calcium on lipid metabolism
① Large amount of dietary calcium in the extracellular environment
② Inhibition of the parathyroid hormone and the active form of vitamin D (1,25-hydroxy vitamin D).
③ Inhibition of calcium entry in fat cells
④ The lack of calcium in fat cells enhance fat degradation and inhibit fat synthesis
Additionally, calcium can naturally limit fat absorption. This represents the second advantage of calcium for weight management. This phenomenon has been shown with micellar caseins through a study in 2015. During this study, overweight subjects had to consume a high fat meal with a portion of proteins. It could be caseins, classic whey or whey enriched in α-lactalbumine. Analyses have shown a significant average decrease of 22% of fat absorption with caseins. 8 A second study in 2001 has also shown that a consumption of calcium of 900mg/d could multiply lipid excretion by 2, and decrease LDL cholesterol concentration (commonly called “bad cholesterol”) by 15% after only 2 weeks of supplementation. 9
Moreover, calcium would, in the same way as proteins, increase thermogenesis and therefore increase energy expenditures. 2 10
Are micellar caseins more interesting than a calcium supplement?
Micronutrients (vitamins and minerals) found directly in food are generally better absorbed by the body than those provided in free form via a food supplement. Therefore, calcium from micellar caseins should be absorbed much better. 2 3 11 12 13
Furthermore, caseins represent a good calcium source with approximately 2,600mg/kg 14 , but also a very good source of interesting proteins for weight loss. It is better to combine the entire factors which enhance weight management rather than consider an isolated element, such as calcium alone. This was particularly highlighted in the previously cited 2019 study. 5
What about whey proteins? Is it of particular interest?
Yes, it is a particularly interesting protein for its short-term satietogenic effect. Compared to other protein sources, whey proteins are very efficient to quickly increase the feeling of fullness. Therefore, this favors the reduction of food intakes. 15 16
Furthermore, certain studies have observed a reduction of postprandial (after a meal) blood glucose when whey proteins are consumed before a high carbohydrates meal. This has been shown in a 2010 study in which one healthy subjects had consumed different amounts of whey before a meal (between 10 and 40g), after which blood glucose was measured. Then, authors noted that the more whey protein is consumed before meal, the least blood glucose was (maximal effect for 40g of whey proteins) 17. This can be very interesting; especially for people having difficulties in regulating their food intake or overweight subjects who want to reduce their energy consumption.
Therefore, micellar caseins or whey proteins can represent interesting proteins for weight management.
For more information, contact us.
Authors: Rémi Maleterre & Audrey Boulier.
_______________________________________________________________________________________________
[1] « Obesity and overweight». World Health Organization. WHO. February 16, 2018 [consulted: july 09, 2019]. https://www.who.int/news-room/fact-sheets/detail/obesity-and-overweight
[2] D. Paddon-Jones, E. Westman, R.D. Mattes, R.R. Wolfe, A. Astrup, M. Westerterp-Plantenga (2008). Protein, weight management, and satiety. The American Journal of Clinical Nutrition, Volume 87, Issue 5, May 2008, Pages 1558S–1561S. Pub May 01, 2008. https://doi.org/10.1093/ajcn/87.5.1558S
[3] S. Schrager (2005). Dietary Calcium intake and obesity. J Am Board Fam Pract. 18(3):205-10. Pub May 2005.
[4] M. Van Loan (2009). The role of dairy foods and dietary calcium in weight management. Journal of the American College of Nutrition. 28:supp1, 120S-129S. Epub June 14, 2013. https://doi.org/10.1080/07315724.2009.10719805
[5] J.Z. Ilich, O.J. Kelly, P.Y. Liu, H. Shin, Y. Kim, Y. Chi, K. Wickrama, I. Colic-Baric (2019). Role of Calcium and low-fat dairy foods in weight-loss outcomes revisited: results from the randomized trial of effects on bone and body composition / obese postmenopausal women. Nutrients 2019, 11(5), 1157. Epub May 23, 2019. https://doi.org/10.3390/nu11051157
[6] M.B. Zemel (2003) Mechanisms of dairy modulation of adiposity. J Nutr 2003;133:252S–6S. Pub January 2003. https://doi.org/10.1093/jn/133.1.252S
[7] M.B. Zemel (2002). Regulation of adiposity and obesity risk by dietary calcium: mechanisms and implications. J Am Coll Nutr 2002;21:146S–51S. Pub April 2002.
[8] F. Mariotti, M. Valette, C. Lopez, H. Fouillet, M.H. Famelart, V. Mathé, G. Airinei, R. Benamouziq, C. Gaudichon, D. Tomé, D. Tsikas, J.F. Huneau (2015) Casein compared with whey proteins affects the organization of dietary fat during digestion and attenuates the postprandial triglyceride response to a mixed high-fat meal in healthy, overweight men. J Nutr 145, 2657–2664. Pub December 2015. https://doi.org/10.3945jn.115.216812
[9] Y. Shahkalili, C. Murset, I. Meirim, E. Duruz, S. Guinchard, C. Cavadini, K. Acheson (2001) Calcium supplementation of chocolate: effect on cocoa butter digestibility and blood lipids in humans. Am J Clin Nutr 2001;73:246 –52. Pub February 2001. https://doi.org/10.1093/ajcn/73.2.246
[10] H. Shi, A.W. Norman, W.H. Okamura, M.B. Zemel (2001). 1alpha25-Dihydroxyvitamin D3 inhibits uncoupling protein 2 expression in human adipocytes. FASEB J 2002;16:1808 –10. Pub December 2001. https://doi.org/10.1096/fj.01-0584fje
[11] M. Zemel, W. Thompson, A. Milstead, K. Morris, P. Campbell (2004). Calcium and dairy acceleration of weight and fat loss during energy restriction in obese adults. Obes Res 2004;12:582–90. Pub April 2004. https://doi.org/10.1038/oby.2004.67
[12] Ingredia. Prodiet 87 B Fluid – Nutrition facts . December 11, 2015.
[13] B.L. Luhovyy, T. Akhavan, G.H. Anderson. (2007). Whey proteins in the regulation of food intake and satiety. Journal of the American College of Nutrition, Vol 26, Issue 6, p704S-712S. Epub June 14, 2013. https://doi.org/10.1080/07315724.2007.10719651
[14] S. Pal, S. Radavelli-Bagatini, M. Hagger, V. Ellis. (2014). Comparative effects of whey and casein proteins on satiety in overweight and obese individuals: a randomized controlled trial. European Journal of Clinical Nutrition. 68, 980-980. Epub May 07, 2014. https://doi.org/10.1038/ecjn.2014.84
[15] T. Akhavan, .L. Luhovyy, P.H. Brown, C.E. Cho, G.H. Anderson (2010). Effect of premeal consumption of whey protein and its hydrolysate on food intake and postmeal glycemia and insulin responses in young adults. The American Journal of Clinical Nutrition, Volume 91, Issue 4, April 2012, 966-975. Epub April 4, 201. https://doi.org/10.3945/acjn.2009.28406
Fighting undernourishment in hospitals
Undernourishment affects more than 50% of patients with cancer or Alzheimer’s disease in France. It may unfortunately worsen with therapeutic management and results in increased morbidity (i.e. amplify disease) and death.
These statistics have remained unchanged for 30 years because the assessment of the patient’s nutritional status is rarely carried out. In order to bridge these nutritional deficiencies in hospitals, it is important to provide adequate nutritional supplements.1 2
What is undernourishment?
Undernourishment corresponds to an imbalance between nutritional intake and the body’s needs. This can have important consequences, such as organs dysfunction or the loss of certain tissues, especially muscles. The first alarming symptom will be an important weight loss.2 3
When undernourishment becomes too important, then we have cachexia: a profound weakening of the body characterized by a significant loss of muscle mass, a deficient immune system, and a decrease in cognitive and physical abilities.4
Why is the number of undernourished patients so high?
There are several possible explanations for this high number of undernourished patients, particularly those with cancer.
First, it is not uncommon for cancer patients not to eat enough. Consequently, energy providings are inferior to the bodily needs. Causes can be multiple. The disease or the treatment may cause hormonal disturbances affecting hunger signals, or have an important psychological impact on the patient who can lose their appetite. 5
Secondly, almost one-third of cancers affects digestive organs (colon and rectum, liver, pancreas,…) and elimination organs (renal system, bladder). This can lead to dysfunctions in the digestive system and then malabsorption or misuse of certain nutrients.3 6
Finally, in the case of cancers, tumor consumes a lot of energy at the expense of the integrity of the body. Therefore, it is essential for the patient to consume a sufficient amount of energy and essential nutrients so as not to increase deficiencies.4 7
What are the most common nutritional deficiencies in these patients?
The first nutritional deficiency that may show visible side effects is the lack of proteins. The protein need is about 0.8g/kg of bodyweight per day.8 9
Protein deficiency exists when the subject does not consume enough proteins to meet his needs (so less than 0.8g/kg/d) or when an essential amino acidA is deficient. That is why hospitalized patients, who consume less food and/or do not assimilate them as well, are much more exposed to a lack of protein.10
The deficiency of one or more essential amino acids is also amplified if the person does not consume enough proteins of good quality and if sources are not suitably varied. For more information on the quality of proteins, see our article “How to characterize the quality of a protein”.
To synthetize muscles, our body needs all essential amino acids. This synthesis will then be proportional to the nutritional intake of the most deficient amino acid called limiting amino acid. In other words, if the requirements for the limiting amino acid are only covered up to 30%, then anabolismB will only reach 30% of its potential. As shown in Figure 1, the deficiency of a single essential amino acid is sufficient to unbalance the protein balance.11
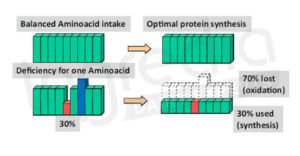
Figure 1: Effect of a lack of one essential amino acid on body protein synthesis.9
A chronic imbalance in protein intake can lead to a progressive loss of muscle mass accompanied by a decrease in physical strength.1 2 4 But this is not the only risk of muscle mass decrease. It can also lead to a gradual decrease in the proper functions of immune system due to the need of amino acids. This would lead to an increase in morbidity and risk of serious infection, and death (figure 2).12 13
Therefore, an adequate diet and especially a sufficient protein intake is vital for these patients.
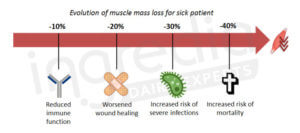
Figure 2: Impact of muscle mass loss for sick patient.12 13
Shouldn’t we consume more proteins to make sure we do not run out of amino acids?
Indeed, we often consider the value of 0.8g of proteins per kg of bodyweight per day. However, for a patient affected by a disease such as cancer, it is recommended to consume more proteins. Based on current scientific knowledge, it has been shown that a consumption of at least 1.2 to 1.6g/kg/d of high-quality proteins appears to be the ideal intake for optimal health in diseased adults.2 8 14
Furthermore, a 2009 clinical study has tried to find a link between nutrition and mortality reduction in critically ill patients. It has been shown that an increase in energy intake of an average of 1034kcal with 47g of proteins per day can significantly reduce the risk of death in undernourished patients or in important weight loss situation (figure 3).15
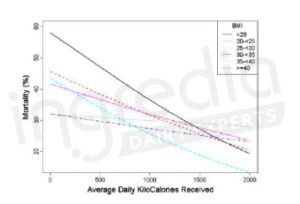
Figure 3: Relation between daily intake (including 18% of proteins) and 60-day mortality expressed with the BMI (Body Mass Index).15
Moreover, other studies have shown a strong correlation between increasing energy consumption (> 1.2 g/kg/d) and the improvement of the health status in sick patients, resulting in a mortality reduction. 7 13 16
What can be the solution to adequately meet the nutritional needs of these patients?
There are two solutions to better cover the nutritional needs of these patients.
The first one is simply to enrich the diet. The aim is then to increase the energy and protein intake without increasing the food volume too much. In order to do this, different products can be used, such as milk powder (whole milk, whey or casein), whole condensed milk, grated cheese, eggs, peanut butter, cream, oil and butter. These foods represent either a high caloric load, especially in the case of fatty foods, or a concentrate of essential nutrients, in the case of eggs and milk products. 17
Unfortunately, enriching the diet is often insufficient to meet nutritional needs of the patient, more particularly in older subjects.18 This is the reason why it is possible to consider an oral nutritional supplement. Then we bring high-calories nutritional supplements and especially rich in proteins and micronutrients (vitamins and minerals) in order to fight against malnutrition. These products are easy and fast to assimilate and can be adapted to the patient tastes: drink, dessert cream, soup, etc… The French National Authority for Health (HAS) recommends the prescription of hyper-energetic and/or hyper-protein products to achieve a dietary supplement of 400kcal/d and/or 30g of proteins per day, most often with 2 products per day.19 20
What kind of proteins is contained in these oral nutritional supplements?
These products often contain micellar caseins because they are complete proteins that can meet the nutritional needs of undernourished people. Moreover, they are ideal for the formulation of drinks or dessert creams because they are resistant to heat treatments and they allow for the conservation of the desired texture of the product.21
For more information, please contact us
Authors: Rémi Maleterre & Audrey Boulier.
*A [Essential Amino Acids]: Amino acids the body cannot synthesize. Therefore they must be supplied through the diet.
*B [Anabolism]: Muscular protein synthesis.
_________________________________________________________________________________________
[1] S. Benoist, A. Brouquet (2015). Dépistage de la dénutriton. Nutritional assessment and screening for malnutrition. Journal de Chirurgie Viscérale, 152(1):3-7. Pub February 2015. https://doi.org/10.1016/S1878-
[2] SFNEP (Société Francophone Nutrition Clinique et Métabolisme). « Nutrition chez le patient adulte atteint de cancer ». SFNEP professional recommandation [présentation of november 2012]
[3] P. Shetty (2006). Malnutrition and undernutrition. Medicine, 34(12):524-529. Pub December 2006. https://doi.org/10.1053/j.mpmed.2006.09.014
[4] J.M. Argilés (2005). Cancer-associated malnutrition. Eur J Oncol Nurs. 9(2):S39-50. https://doi.org/10.1016/j.ejon.2005.09.006
[5] Cancer Treatment Centers of America. “Malnutrition” [online] https://www.cancercenter.com/integrative-care/malnutrition. Last accessed September 3, 2019.
[6] American Cancer Society: Cancer Facts and Figures 2019. Atlanta, Ga: American Cancer Society, 2019 [online]. https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2019/cancer-facts-and-figures-2019.pdf Last accessed September 3, 2019.
[7] H.F.R. da Cunha, E.E.M. da Rocha, M. Hissa (2013). Protein requirements, morbidity and mortality in critically ill patients: fundamentals and applications. Rev Bras Ter Intensiva, 25(1):49-55. Pub January 2013. https://doi.org/10.1590/S0103-507X2013000100010
[8] Poortmans, J.R., Carpentier, A., Pereira-Lancha, L.O., & Lancha Jr., A. (2012). Protein turnover, amino acid requirements and recommendations for athletes and active populations. Brazilian Journal of Medical and Biological Research, 45(10), 875-890. Epub June 06, 2012. https://dx.doi.org/10.1590/S0100-879X2012007500096
[9] National agency of food safety, environmend and work (ANSES). (2019) Les protéines : définition, rôle dans l’organisme, sources alimentaires. At: https://www.anses.fr/fr/content/les-prot%C3%A9ines
[10] D.W. Nixon, S.B. Heymsfield, A.E. Cohen, M.H. Kutner, J. Ansley, D.H. Lawson, D. Rudman (1980). Protein-calorie undernutrition in hospitalized cancer patients. The American Journal of Medicine, 86(5): 683-690. Pub May 1980. https://doi.org/10.1016/0002-9343(80)90254-5
[11] M.F. Holick (2003). Vitamin D: a millennium perspective. J Cell Biochem. 1;88(2):296-307. Pub February 1, 2003. https://doi.org/10.1002/jcb.10338
[12] D.W. Chang, L. DeSanti, R.H. Demling (1998). Anticatabolic and anabolic strategies in critical illness: a review of current treatment modalities. Shock, 10(3):155-60. Pub September 1998.
[13] Frebesenius Kabi. « The Role of Protein in critically ill patients » [online]. https://clinicalnutrition.com.ar/en/the-role-of-protein-in-critically-ill-patients/. Last accessed September 6, 2019.
[14] S.M. Philips, S. Chevalier, H.J. Leidy (2016). Protein « requirements » beyond the RDA : implications for optimizing health. Adv. Physiol. Nutr. Metab. 41(5): 565-572. Epub February 9, 2016. https://doi.org/10.1139/apnm-2015-0550
[15] C. Alberda, L. Gramlich, N. Jones, K. Jeejeebhoy, A.G. Day, R. Dhaliwal (2009). The relationship between nutritional intake and clinical outcomes in critically ill patients: results of international multicenter observational study. Intensive Care Medicine, 35(10):1728-1737. Pub July 02, 2009. https://doi.org/10.1007/s00134-009-1567-4
[16] P.J.M Weijs, S.N. Stapel, S.D.W. de Groot, R.H. Driessen, E. de Jong, A.R.J. Girbes, R.J.M. Strack van Schijndel, A. Beishuizen (2011). Optimal Protein and Energy Nutrition decreases mortality in mechanically ventilated, critically ill patients. Journal of Parenteral and Enteral Nutrition, 36(1):60-68. Pub December 13, 2011. https://doi.org/10.1177/0148607111415109
[17] B. Dorner (2009). Fortify to enhance nutritional value. Today’s Dietitian, 11(7):20. Pub July 2009. https://www.todaysdietitian.com/newarchives/062909p20.html
[18] C. Gaillard, E. Alix, Y. Boirie, G. Berrut, P. Ritz (2008). Are elderly hospitalized patients getting enough protein? Journal of the American Geriatrics Society. 56(6):1045-1049. Pub June 02, 2008. https://doi.org/10.1111/j.1532-54152008.01721
[19] I. Bourdel-Marchasson, M. Barateau, V. Rondeau, L. Dequae-Merchadou, N. Salles-Montaudon, J.P. Emeriau, G. Manciet, J.F. Dartiques (2000). A multi-center trial of the effects of oral nutritional supplementation in critically ill older inpatients. Nutrition, 16(1):1-5. Pub January 2000. https://doi.org/10.1016/s0899-9007(99)00227-0
[20] HAS (French National Authority for Health). « Synthèse des recommandations professionnelles (2007) ». Stratégie de prise en charge en cas de dénutrition protéino-énergétique chez la personne âgée. [online]. https://www.has-sante.fr/upload/docs/application/pdf/synthese_denutrition_personnes_agees.pdf. Last accessed September 4, 2019.
[21] Ingredia, Prodiet Fluid. The Innovative Micellar Casein dedicated to high protein beverages. [online] https://www.prodiet-fluid.com/. Last accessed September 4, 2019
The role of proteins in enteral nutrition
Enteral nutrition replaces the oral intake of food and drink and is the process of feeding by tube directly into the stomach. It is also known as tube feeding.
The tube is passed through the nose or mouth into the stomach as a short-term feeding solution and can be used intermittently with oral feeding. For long-term patient care, tubes are inserted into the stomach or small intestine. Enteral nutrition can only be used when the gut is working correctly and can absorb the nutrients.
This form of feeding is a quick and efficient way to deliver protein and other nutrients to patients who are critically ill, suffer from a chronic disease or are malnourished or protein deficient.

When are proteins used in enteral nutrition?
Liquid protein is used in enteral nutrition when a patient is unable to feed by mouth or needs extra protein, carbohydrates, fat, water and other nutrients.
Tube feeding occurs for several reasons, depending on the situation. This includes muscle deterioration in critically ill patients, as muscles begin to waste when they are not used. This can be a problem for patients who survive or endure a long-term critical illness as muscles can take several years to repair, particularly if the patient is no longer active.
Using liquid protein in enteral nutrition can assist with muscle repair.
Products are formulated using different volumes of the source nutrients, which can be administered depending on the patient’s needs.
Protein sources for enteral nutrition products include milk protein, whey protein, caseins and soy protein.
Protein-rich formulas can also be developed to address specific diseases and medical situations, for example, high protein products can promote wound healing.
Why is protein used in enteral nutrition?
Protein can be delivered to the body fast by way of enteral nutrition. This is particularly important when patients are undergoing critical care. The body needs protein to repair and survive and cannot function without it.
With tube feeding, the amount of protein intake can be controlled to ensure the correct quantity is absorbed.
Common situations requiring protein-supplemented enteral nutrition include:
- After operations on the face, neck, throat, gullet or stomach
- Strokes or other neurological conditions causing swallowing to be
difficult or impossible
- After radiotherapy to the throat
- When there is a stomach blockage

Both whey and casein-based protein products can be used to tube-feed critically ill patients. The body absorbs whey at a faster rate than casein. Sometimes both ingredients are combined to obtain a particular nutritional composition.
Casein is beneficial to muscle restoration as it is slowly absorbed and can work continuously over a long recovery period, particularly when a patient has limited mobility. Casein is also a high-quality protein delivery method derived from cow’s milk, and is considered to be more efficient than vegetable protein.
However, some studies have shown that whey protein is better able to stimulate the initial muscle restoration process. This is because the amino acid, leucine, is the substance that triggers the process and whey protein contains more leucine than casein.
Therefore, whey promotes muscle restoration and casein enhances it.
Casein-based protein formulas are also commonly used when coagulation is required to encourage the body to retain and absorb nutrients.
Proteins play an essential role in enteral nutrition, alongside other ingredients required to provide patients with the right balance of nutrients. Different formulations are developed according to/depending on patients’ specific nutritional requirements.
For any other inquiry, contact us.
________________________________________________________________________________________________
Sources:
Burrin, D. G. (2004). Proteins and amino acids in enteral nutrition. PubMed. https://pubmed.ncbi.nlm.nih.gov/15090907/
https:\/\/dietitiansondemand.com\/enteral-nutrition-overview-formula-selection-considerations\/#author. (2020, December 17). Enteral Nutrition Overview + Formula Selection Considerations. Dietitians On Demand | Professional Recruiting Services for Contract and Permanent-Hire Positions. https://dietitiansondemand.com/enteral-nutrition-overview-formula-selection-considerations/
Reinhold, S. (2020, August 25). Protein delivery in intermittent and continuous enteral nutrition with a protein-rich formula in critically ill patients—a protocol for the prospective randomized controlled proof-of-concept Protein Bolus Nutrition (Pro BoNo) study. Trials. https://trialsjournal.biomedcentral.com/articles/10.1186/s13063-020-04635-1
Savino, P. (2018, February 1). Knowledge of Constituent Ingredients in Enteral Nutrition Formulas Can Make a Difference in Patient Response to Enteral Feeding. American Society for Parenteral and Enteral Nutrition. https://aspenjournals.onlinelibrary.wiley.com/doi/full/10.1177/0884533617724759
van de Walle, M. G. S. (2021, June 16). What Is Casein, and Does It Aid Muscle Growth? Healthline. https://www.healthline.com/nutrition/what-is-casein#bottom-line
The importance of high protein and high-calorie products in clinical nutrition and their effect on cancer, kidney problems, and metabolic syndrome
Protein is essential for good health. The body cannot survive without protein – it promotes tissue and muscle growth and repair, and can help boost the immune system.
However, during illnesses such as cancer, kidney disease and metabolic syndrome 2, extra protein and calories are sometimes required. This can be due to a loss of appetite or an inability to absorb the amount of protein and calories the body needs. When a person does not feel like eating or cannot eat properly, protein and calories can be supplied through beverages and desserts made with the milk protein, micellar casein.

Is nutritional intervention helpful in cancer patients?
Cancer patients, in particular those undergoing chemotherapy, tend to lose their appetite which results in a loss of energy and weight. This is known as a decrease in HRQoL (health-related quality of life). Without nutritional intervention, this can result in a vicious circle as the body needs to be strong to deal with the effects of chemotherapy.
To support this theory, a study by Sophie C. Regueme et al. carried out in 20201 , investigated the effect of nutritional intervention on 155 older cancer patients. A decline in daily living activity and an increase in fatigue was seen due to low protein intake. The addition of supplementary protein in the diet showed an improvement in these symptoms.
Nutritional drinks and desserts can be ideal for patients receiving cancer treatment as they are a convenient source of protein and calories. They are easy to consume between meals or as a replacement. It should be noted that it is also important for cancer patients to try and eat a light balanced diet when possible, to maintain the correct nutritional balance.
What are the effects of dietary protein on kidney function?
A high-protein diet may be a contributing factor to chronic kidney disease and a low-protein diet is recommended. This is because too much protein can cause extra waste to form in the blood and the kidneys may not be able to expel it.
However, in kidney dialysis (when the blood is cleaned in a machine because the kidneys are not functioning properly) patients can benefit from extra protein. This is because as well as filtering out the harmful waste, dialysis also removes a substance called albumin. Albumin is a form of protein that makes up about 60% of the blood and transports vitamins, minerals, nutrients and energy around the body. It also helps fluid remain in the blood vessels.
During dialysis, albumin levels drop and so do not do their job correctly. Therefore, albumin levels should be increased, which can be done through supplementary drinks that are high in protein.

Does protein supplementation benefit patients with metabolic syndrome?
Metabolic syndrome is a group of conditions that occur together: diabetes, high blood pressure, and obesity. It affects the blood vessels and, if left untreated, can lead to cardiovascular disease and stroke. According to the NHS (National Health Service), one in three people over 50 in the UK suffer from metabolic syndrome.
Protein can improve resistance to the body’s chemical insulin, which is a common complication of obesity. This can lead to type 2 diabetes, which is a chronic condition that has no cure. Most people with type 2 diabetes have to take medicine throughout their lives to manage their blood sugar levels.
Metabolic syndrome can be prevented or assisted with the help of increased protein intake. Studies have been carried out to show that dairy components, such as whey proteins and casein, may contribute to a reduction in the risk of developing metabolic syndrome. For this reason, high protein drinks and desserts made with the protein PRODIET® Fluid can be beneficial for people with metabolic syndrome.
From the research carried out, it can be seen that products made with a high protein and high calorie content can be beneficial for cancer, kidney dialysis and metabolic syndrome sufferers. As a functional and nutritional high-quality protein, PRODIET® Fluid is a suitable ingredient for the manufacture of nutritional beverages and drinks which can supplement dietary needs.

For any other inquiry, contact us.
________________________________________________________________________________________________
Sources:
[1] Sophie C. Regueme et al., 2020 Protein intake, weight loss, dietary intervention, and worsening of quality of life in older patients during chemotherapy for cancer https://pubmed.ncbi.nlm.nih.gov/32435967/
[2]https://www.nhs.uk/conditions/metabolic-syndrome/
[5] Gang Jee Ko et al., 2017 Dietary Protein Intake and Chronic Kidney Disease https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5962279/#:~:text=High%20protein%20intake%20may%20lead,for%20the%20management%20of%20CKD.
The importance of high protein/high-calorie products in clinical nutrition
The right protein and calorie intake are essential for good health. However, some people with gastric problems that affect the stomach and intestines find it difficult to obtain the amount of protein and calories their body needs through a normal diet.
Protein and calorie-enriched products can aid digestion and help ensure the body receives enough of these minerals to function healthily.
What is clinical nutrition?
Clinical nutrition is the medical term used to advise patients on how to eat correctly to maximise health, especially if they suffer from chronic disease. Gastrointestinal disorders are a particularly common problem that can be treated with careful management of nutritional intake and are linked to the body’s inability to process certain substances.
According to a study carried out by the University of Gothenburg, 4 out of every 10 adults in the world suffer from a gastric disorder. Clinical nutrition is a way to prevent and manage these disorders by the consumption of additional protein or calories, as required.

What are the most common gastroenteropathy conditions?
Problems with the gastrointestinal tract can present in a variety of conditions, including:
- indigestion
- heartburn
- acid reflux
- constipation
- stomach bloating
- irritable bowel syndrome (IBS)
These can occur at any time in a person’s life and the correct clinical nutrition advice can help ease and treat the symptoms.
These disorders can be the result of a busy, stressful lifestyle when sometimes people don’t find the time to eat a regular, healthy meal.
The symptoms are also often linked to poor digestion, which is essential for the body to absorb the nutrients provided by food and drink, including protein and calories.

What are the benefits of high protein/high-calorie products on gastrointestinal disorders?
Whilst many people need to follow a high-protein or high-calorie diet to ensure their intake is right for them, it can be difficult to digest some foods, which can lead to the above conditions.
The body needs to digest protein in the natural form of foods such as eggs, lean meat, fish, seafood and dairy products. An alternative to these is protein supplements or foods and drinks made with added protein. The protein turns into amino acids which are absorbed into the blood through the intestines and carried into the body.
Stomach acid promotes enzymes in the body to break down protein before it is absorbed. We cannot absorb protein simply by eating protein-filled foods – the breakdown process is essential.
But some people do not have the right enzymes to process proteins in certain foods. This is especially common in older people as the stomach produces fewer enzymes as we age.
If the body cannot tolerate certain foods, it can be impossible to achieve the right nutritional intake.
Protein-enriched products such as desserts and ready-to-drinks containing extra protein or calories can be the ideal way to get the correct intake of these nutrients without upsetting the stomach.
These foods and drinks are also beneficial for people who suffer from gastric problems. They are convenient and easy to consume while working or after exercising and are a suitable alternative to skipping meals.
Another benefit of high-protein foods is that they make you feel full for longer, indicating the right number of calories has been consumed. This helps prevent the desire to snack on unhealthy foods that the body may not be able to tolerate.
Protein and calorie-enriched products are also beneficial for older people who find it difficult to eat large meals. As we age our metabolic rate changes and appetite often reduces. This loss of appetite can be due to certain health conditions, or simply the results of old age.
However, it is still important for older people to eat the right foods in the correct amounts. An instant soup, a creamy dessert or a high protein/high calorie drink can be much more appealing to an older person than a large meal.
Therefore, foods and drinks with added protein are beneficial for people with gastrointestinal problems as a form of diet control.

For more information and any inquiry, contact us.
_________________________________________________________________________________________
Sources:
https://pubmed.ncbi.nlm.nih.gov/23567359/:
Dietary proteins and functional gastrointestinal disorders. (2013). National Library of Medicine. https://pubmed.ncbi.nlm.nih.gov/23567359/
Study shows global prevalence of functional gastrointestinal disorders. (2020). News Medical Life Sciences. https://www.news-medical.net/news/20200527/Study-shows-global-prevalence-of-functional-gastrointestinal-disorders.aspx#:~:text=For%20every%20ten%20adults%20in,those%20now%20presenting%20these%20results.
https://www.healthline.com/health/protein-digestion:
Dix, R. M. N. (2021, April 1). How Is Protein Digested? Healthline. https://www.healthline.com/health/protein-digestion
https://www.niddk.nih.gov/health-information/digestive-diseases/digestive-system-how-it-works:
Your Digestive System & How it Works. (2021, July 7). National Institute of Diabetes and Digestive and Kidney Diseases. https://www.niddk.nih.gov/health-information/digestive-diseases/digestive-system-how-it-works
WHY IS NUTRITION IMPORTANT FOR PEAK ATHLETIC PERFORMANCE?
The correct nutritional balance can assist and enhance athletic performance. Just as a performance car engine needs the right fuel and oil to run at its best, athletes can optimise their performance with the right nutritional intake.
Athletes need higher protein levels than the average person to maintain energy levels, muscle growth and repair. The amount of extra protein an athlete requires depends on their body composition, weight and the type of sport they practise.

Why do athletes use protein supplements?
Exercise can cause muscle damage and muscles need protein to grow and repair. Athletes often use protein supplements in their diet to promote this repair as this is a convenient way to increase protein intake. It’s easy to consume a protein shake or bar either pre-training or after, especially if the athlete doesn´t have the time to eat a protein-enriched meal at this time.
The amount of protein an athlete needs depends on the type of sport or training they do. For example, a runner (endurance) will need a different amount than someone who performs weight training (resistance).
Another benefit of protein supplements is that they can speed up muscle repair. During exercise muscles can tear, even minutely, and protein helps these tears to repair quickly.
Some athletes also take protein supplements to help injuries heal faster. For professional athletes, this is essential, as long-term muscle injuries can equal a loss of career development.
What is an athletes’ typical nutritional intake?
Athletes take sports nutrition seriously and have to plan their protein and carbohydrate intake and adjust their meals and snacks depending on their activity. This takes discipline, which comes from the desire to succeed in a particular sporting field.
The RDA (recommended daily allowance) of protein is 0.8 grams of protein per kilogram for the average person. According to the British Nutrition Foundation, strength and endurance athletes need around 1.2-2.0 grams of protein per kilogram of bodyweight.
In addition to a high-protein diet that includes red meat, chicken, fish, dairy products, eggs and nuts, milk-based protein supplements deliver a further source of protein. In the form of protein drinks, snacks and powders, these products offer athletes a suitable alternative to consuming more protein through eating extra meals.
Milk is another athletes’ favourite for recovery after a training session or event as it contains a balance of protein and carbohydrates. It also includes whey protein (which the body absorbs quickly) and casein (which absorbs more slowly), the combination of which increase muscle repair and energy levels.

Why is sports nutrition planning essential for athletes?
The timing of protein intake for athletes is crucial – it’s easier on the stomach to consume a protein supplement before an event or training than to eat a large, protein-fuelled meal.
Just as important is post-sports nutrition, and many athletes take protein supplements after activity to replenish energy levels and prevent muscle soreness. Plus, drinking a protein shake or eating an energy bar is easier than eating a big meal directly after training.
Milk-based proteins are particularly useful for this as they prompt the fast growth of muscle mass. A study carried out by the Journal of Nutrition concluded “The results suggest that high protein and dairy intake led to the best results in terms of weight loss and muscle gain.”
Muscle mass is the amount of muscle in the body. Not only does muscle mass contribute to a lean appearance, but it’s also beneficial for a healthy body as it can help boost the immune system, regulate glucose levels and aid illness recovery.
Timing is essential also in sports nutrition during low-intensity periods. To maintain the right balance, athletes adjust the amount of protein (and carbohydrates and fat) they receive daily depending on whether their training is light or high-intensity. This adjustment is essential out of season when athletes are only training and not performing.

What’s the future for sports nutrition?
There is increasing demand for sports nutrition products for athletes that are convenient, taste good and benefit performance. Research carried out by Allied Market Research expects the sports nutrition market to grow to $44,003 million this year.
This is an opportunity for sports nutrition manufacturers to also grow sales by offering quality products to cater for the needs of athletes, fitness enthusiasts and the general sports market.
For any other inquiry, contact us.
________________________________________________________________________________________________
Sources:
http://www.sportsnutrition2win.com/uploads/7/0/2/5/70257083/recovery.pdf
https://www.medicalnewstoday.com/articles/323093
https://jissn.biomedcentral.com/articles/10.1186/s12970-018-0242-y
https://www.alliedmarketresearch.com/sports-nutrition-market
https://www.verywellfit.com/milk-protein-superior-for-muscle-growth-3984402
Why should you choose Ingredia’s Prodiet® milk proteins?
Over the past few decades, interest in animal welfare has grown steadily. In August 2020, the IFOP (French Institute of Public Opinion) published a survey conducted for the Brigitte Bardot Foundation (French Foundation dedicated to animal protection) on the opinion of French regarding the animal condition. Out of a sample of 1009 people, more than 4 out of 5 persons are in favor of a prohibition on breeding animals in conditions that do not meet their needs, i.e. in closed buildings without outside access. However, in France, 4 out of 5 animals are bred under these conditions…1

How can we fight against these farming methods?
The best way is to adopt a more responsible consumption pattern: consume products made with respect for the environment and animal welfare is the best choice to encourage this sector to develop better!
In the case of milk and dairy ingredients, it is making the choice of Ingredia and milk cooperative such as Prospérité Fermière!
What are the commitments of milk from Prospérité Fermière cooperative?
The Prospérité fermière commits to product sustainable milk through the Via Lacta approach. It is based on 3 points: Humans, Milk and Environment.
In the introduction of this article, we talked about breeding in closed buildings: with Via Lacta milk, respect for the living conditions of cows is at the heart of concerns. This is the reason why cows spend 170 days a year on pasture with at least 1500m² of grass per animal. We are far away from stables and their 10m² per cow.2 This is made possible by the fact that in the Hauts-de-France region, the cooperative has 1600 member-producers from 1000 family-sized farms: with an average of 50 cows, these farms are perfectly compatible with animal welfare.3
In this idea of sustainable development, the Prospérité Fermière has established a differentiating collection program. So, traditional milk and milk from grass-fed cows are only collected within an 80km radius around the St-Pol-sur-Ternoise creamery located in the region of Hauts-de-France. This allows to:
-
- Limit the carbon footprint of milk by reducing transport
- Boost local production while preserving grassy landscapes of the Hauts-de-France region
- Correctly remunerate breeders by fixing a minimum price per year as well as a bonus for the grass-fed milk production.3

From a product quality point of view, is milk from grass-fed cows different from conventional milk?
In addition to the eco-responsible dimension (natural and GMO-free) of promoting grass-fed milk, it is important to know that milk is a reflection of the diet of the cow which produced it.
This was studied during a 2019 review: the purpose was to compare the nutritional quality of milk from grass-fed cows and a more conventional milk. The study revealed that the milking cow’s diet had a direct impact on the fat profile of the milk:4
-
- Milk from Grass-fed cows contains more polyunsaturated fatty acids and less saturated fatty acids, which is positive as it is always better to reduce your saturated fatty acids intake in favor of unsaturated fats.
- Grass-fed milk contains less omega 6 and more omega 3 fatty acids. The nutritional interest of grass-fed milk is therefore superior since our diet is generally too rich in omega 6 and too low in omega 3, whereas it is important to respect a low omega 6/omega 3 ratio.
- Grass-fed milk contains more CLA (conjugated linoleic acid). A 2015 review details the positive health impact of these molecules, such as stimulating the immune system and reducing the risk of cancer and type II diabetes.5 These molecules could also stimulate metabolism, and so on increase energy expenditure. This is the reason why CLA dietary supplements can be found on the market.
A study by the Chamber of Agriculture of Brittany carried out between 2006 and 2008 demonstrates the same results.6 In figure n°1, we can observe that an increase of pasture in forages allows an increase in the proportion of polyunsaturated fatty acids, an increase in the CLA content, as well as a decrease in the omega 6/omega 3 ratio.
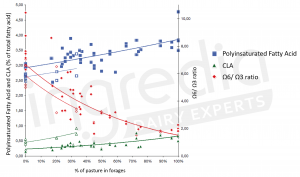
Figure n°1: Evolution of milk composition (polyunsaturated fatty acids, CLA and omega-6/omega-3 ratio) with the part of grass in the cows’ diet.6
Therefore, in addition to more conventional milk, the Prospérité Fermière cooperative offers this eco-friendly grass-fed milk of greater nutritional quality. Moreover, some of the Ingredia’s dairy ingredients come from this special collection milk.
Concerning dairy ingredients, why should we choose Ingredia?
The first important point is the quality of raw materials. Not all products in the dairy ingredients industry come directly from milk. Some come from co-products of other industries. For example, it is possible to use whey from cheese industry. However, proteins of this whey are usually broken down by different thermal or chemical treatments that may be done during the cheese production. Whey proteins from cheese are produced from these whey proteins.
But if a protein is denatured, it can lose some of its bioactive properties.
Concerning Ingredia’s dairy ingredients, this is not the case: the raw material is milk; therefore, ingredients are native and not broken down (native whey proteins, micellar caseins).
But in the case of casein ingredients, the raw material is necessarily milk. So they all use “native” caseins, don’t they?
No, they don’t, as shown in figure n°2 there are 2 types of caseins:
-
- Micellar caseins: they are obtained by membrane filtration. So, proteins are not denatured and keep their native structure.
- Caseinates: they are obtained by a denaturing chemical process.
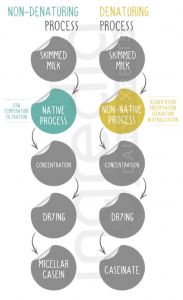
Figure n°2: The 2 processes to obtain caseins from skim milk.7
In order to preserve all caseins properties, Ingredia promotes membrane filtration, a non-denaturing physical process, and offers different micellar caseins with different functional properties depending on the application.
To summarize, Via Lacta is part of a global approach. All actors of the milk production commit themselves to respect a highly controlled specifications in order to ensure:
-
- Animal welfare
- An eco-responsible milk of the best possible quality
- The correct remuneration of producers
In this same idea of research for the best possible quality, Ingredia is always looking for processes that best preserve the produced ingredients.

For more information, do not hesitate to consult the following links:
- The Prospérité Fermière milk (French website): https://www.lait-prosperite.fr/
- Ingredia’s dairy ingredients : https://www.ingredia.com/fields-of-expertise/functional-nutritional-proteins/innovative-proteins/
For any other inquiry, contact us.
Author: Rémi Maleterre.
________________________________________________________________________________________________
[1] IFOP, “Les Français et la condition animale,” IFOP, accessed September 28, 2020, https://www.ifop.com/publication/les-francais-et-la-condition-animale/.
[2] Jacques Charlery and Yves Sèité, “Bien Être Des Animaux et Des Éleveurs – Les Vaches Ne s’entassent Pas,” Cap Elevage 14 (May 2007): 24–25.
[3] “Notre coopérative – Coopérative Prospérité Fermière,” accessed October 22, 2020, https://www.lait-prosperite.fr/notre-cooperative/.
[4] Mohammad Alothman et al., “The ‘Grass-Fed’ Milk Story: Understanding the Impact of Pasture Feeding on the Composition and Quality of Bovine Milk,” Foods 8, no. 8 (August 2019): 350, https://doi.org/10.3390/foods8080350.
[5] Bo Yang et al., “Review of the Roles of Conjugated Linoleic Acid in Health and Disease,” Journal of Functional Foods 15 (May 1, 2015): 314–25, https://doi.org/10.1016/j.jff.2015.03.050.
[6] Chambre d’agriculture de Bretagne, “Matière Grasse du lait : l’herbe améliore la qualité nutritionnelle des laits,” May 2009, 2.
[7] “La Caséine Micellaire,” Prodiet Fluid – la caséine micellaire dédiée aux boissons hyperprotéinées (blog), accessed September 28, 2020, https://www.prodiet-fluid.fr/la-caseine-micellaire/.